Understanding Bone Marrow Transplant
Bone marrow transplantation, also known as hematopoietic stem cell transplantation, is a specialized medical procedure that replaces damaged or destroyed bone marrow with healthy stem cells. The bone marrow is the spongy tissue inside bones that produces blood cells, including red blood cells that carry oxygen, white blood cells that fight infection, and platelets that help blood clot. When bone marrow fails due to disease, chemotherapy, or radiation therapy, a transplant can restore its ability to produce healthy blood cells. This procedure is a potentially curative treatment for numerous life-threatening conditions including leukemia, lymphoma, multiple myeloma, aplastic anemia, sickle cell disease, and certain genetic disorders.
The evolution of bone marrow transplantation over the past five decades has transformed it from an experimental last-resort treatment into a standard and often curative therapy for many blood cancers and disorders. Modern advances in conditioning regimens, supportive care, graft-versus-host disease prevention, and infection management have dramatically improved outcomes and reduced treatment-related mortality. Today, leading transplant centers worldwide report long-term survival rates of 60 to 80 percent or higher depending on the disease, disease stage, patient age, and donor type. These improvements have also expanded the eligible patient population, with reduced-intensity conditioning protocols now enabling transplantation in older patients and those with comorbidities who would not have been candidates for traditional full-intensity transplant.
The cost of bone marrow transplantation in the United States is among the highest of any medical procedure, ranging from $350,000 for autologous transplants to over $800,000 for allogeneic transplants when all associated costs are included. These expenses encompass pre-transplant evaluation and conditioning, the transplant procedure itself, extended hospitalization that can last three to six weeks, infection prophylaxis and treatment, blood product support, graft-versus-host disease management, and long-term follow-up. For many patients and families, these costs create an impossible financial burden even with insurance coverage. International transplant centers in countries like Turkey, India, and South Korea offer the same life-saving procedures at 50 to 90 percent lower cost, performed by experienced hematologists and transplant teams at JCI-accredited facilities.
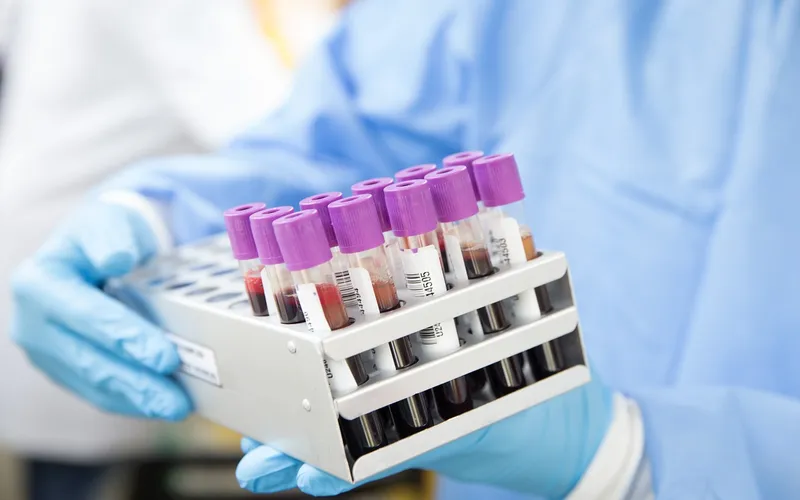
Types of Bone Marrow Transplant
Autologous bone marrow transplant uses the patient's own stem cells, which are collected before high-dose chemotherapy and then reinfused to rescue the bone marrow after treatment. This approach is most commonly used for multiple myeloma, Hodgkin and non-Hodgkin lymphoma, and certain autoimmune conditions. The advantage of autologous transplant is that there is no risk of graft-versus-host disease, since the cells come from the patient's own body. However, the collected cells may contain residual cancer cells, though modern purging and selection techniques have significantly reduced this risk. Autologous transplant is generally better tolerated than allogeneic transplant, with shorter hospital stays and lower complication rates.
Allogeneic bone marrow transplant uses stem cells from a compatible donor, who may be a sibling, parent, unrelated matched donor, or umbilical cord blood donor. This approach is used for leukemias, myelodysplastic syndromes, aplastic anemia, and many other conditions where the patient's own stem cells are diseased or dysfunctional. The key advantage of allogeneic transplant is the graft-versus-disease effect, where the donor's immune cells recognize and attack residual cancer cells in the recipient's body, providing an additional anti-cancer mechanism beyond chemotherapy alone. However, allogeneic transplant carries the risk of graft-versus-host disease, where donor immune cells also attack the recipient's healthy tissues, which can range from mild and manageable to severe and life-threatening.
Haploidentical transplantation is an increasingly important option that uses a half-matched family member as the donor, dramatically expanding the donor pool for patients who lack a fully matched sibling or unrelated donor. With advances in post-transplant cyclophosphamide protocols and other graft-versus-host disease prevention strategies, outcomes with haploidentical donors have improved substantially and now approach those of fully matched transplants for many conditions. Centers like Acıbadem Maslak Hospital and Memorial Şişli Hospital have extensive experience with haploidentical transplantation and can offer this option to patients who might otherwise have no path to transplant. Cord blood transplantation, using stem cells collected from umbilical cord blood after birth, provides another alternative donor source, particularly valuable for patients from ethnic backgrounds underrepresented in international donor registries.
- Autologous transplant — uses patient's own collected stem cells, no GVHD risk
- Allogeneic matched sibling — uses HLA-matched brother or sister, best donor option
- Allogeneic matched unrelated donor — identified through international donor registries
- Haploidentical transplant — uses half-matched family member with specialized protocols
- Cord blood transplant — uses stem cells from donated umbilical cord blood
- Reduced-intensity conditioning — gentler preparation suitable for older or frailer patients
- Tandem autologous transplant — two sequential autologous transplants for high-risk disease
Cost Comparison by Country
The financial burden of bone marrow transplantation is one of the most significant barriers to treatment for patients worldwide. In the United States, the average cost of an autologous bone marrow transplant ranges from $350,000 to $500,000, while allogeneic transplants can cost $500,000 to $800,000 or more when factoring in extended hospitalization, complications management, and post-transplant care. These figures represent the total cost of care from pre-transplant evaluation through the first hundred days post-transplant, which is the most intensive phase of recovery. Additional costs for long-term follow-up, chronic graft-versus-host disease management, and infection prevention can add significantly to the total financial burden over subsequent years.
Bone Marrow Transplant Cost Comparison 2025
| Country | Autologous BMT | Allogeneic BMT | Savings vs USA |
|---|---|---|---|
| USA | $350,000 - $500,000 | $500,000 - $800,000 | — |
| Turkey | $50,000 - $80,000 | $80,000 - $150,000 | Up to 80% |
| India | $25,000 - $50,000 | $40,000 - $80,000 | Up to 90% |
| South Korea | $100,000 - $180,000 | $150,000 - $280,000 | Up to 65% |
| Thailand | $40,000 - $70,000 | $60,000 - $120,000 | Up to 85% |
| Germany | $150,000 - $250,000 | $200,000 - $400,000 | Up to 50% |
| Spain | $120,000 - $200,000 | $180,000 - $350,000 | Up to 55% |
| Singapore | $100,000 - $180,000 | $150,000 - $300,000 | Up to 65% |
Prices include conditioning, transplant procedure, hospital stay, and initial follow-up. Donor search and HLA typing costs may be additional for allogeneic transplants.
Turkey has established itself as a leading destination for bone marrow transplantation, with costs ranging from $50,000 to $80,000 for autologous transplants and $80,000 to $150,000 for allogeneic procedures. These prices represent savings of 70 to 80 percent compared to US costs while maintaining comparable clinical outcomes. Acıbadem Maslak Hospital operates one of the largest bone marrow transplant programs in the region, with HEPA-filtered laminar flow rooms, dedicated transplant nursing staff, and comprehensive supportive care capabilities including access to irradiated blood products, broad-spectrum antimicrobial therapy, and total parenteral nutrition when needed.
India offers the most affordable bone marrow transplant options globally, with prices starting at $25,000 for autologous procedures at centers such as Apollo Gleneagles Hospital. Despite the lower costs, Indian transplant centers have achieved outcomes comparable to international benchmarks, performing thousands of procedures annually with experienced teams. South Korea's Asan Medical Center provides another excellent option, particularly for patients seeking Asian donor compatibility, with one of the largest transplant programs in the Asia-Pacific region and access to extensive donor registries.
Need a bone marrow transplant? Get quotes from world-class transplant centers and find the right treatment plan for your condition.
Get Free Quote
Top BMT Centers Abroad
Choosing the right bone marrow transplant center is a decision that can significantly impact treatment outcomes and long-term survival. The ideal center should have a high annual transplant volume, experienced multidisciplinary teams including hematologists, transplant physicians, specialized nurses, and supportive care specialists, advanced laboratory capabilities for HLA typing and engraftment monitoring, and HEPA-filtered isolation rooms to protect immunocompromised patients. Acıbadem Maslak Hospital meets all these criteria, operating a comprehensive BMT program that handles both autologous and allogeneic transplants for adult and pediatric patients, with particular strength in haploidentical transplantation and treatment of complex hematological malignancies.
Anadolu Medical Center, with its Johns Hopkins Medicine partnership, brings American-standard protocols to Turkey's bone marrow transplant landscape. The center's affiliation ensures adherence to evidence-based guidelines and quality metrics, providing international patients with confidence in the care they receive. Memorial Şişli Hospital rounds out Turkey's premier BMT options with a strong track record in treating both common and rare hematological conditions, a dedicated stem cell processing laboratory, and comprehensive supportive care capabilities that include access to cutting-edge antimicrobial agents, growth factors, and novel immunosuppressive therapies for graft-versus-host disease management.
Donor Matching & HLA Typing
Human leukocyte antigen matching is the cornerstone of successful allogeneic bone marrow transplantation. HLA molecules are proteins found on the surface of nearly all cells in the body that play a crucial role in the immune system's ability to distinguish self from non-self. For bone marrow transplantation, matching at multiple HLA loci between donor and recipient is essential to minimize the risk of graft rejection and graft-versus-host disease. The gold standard is a 10 out of 10 HLA-matched sibling donor, which offers the best outcomes with the lowest risk of complications. However, only about 25 to 30 percent of patients have a fully matched sibling, making alternative donor sources essential for the majority of patients requiring allogeneic transplant.
International donor registries have dramatically expanded the options for patients lacking a matched sibling donor. The World Marrow Donor Association coordinates a global network of registries containing over 40 million potential donors, making it possible to find a matched unrelated donor for many patients. The search process typically takes four to eight weeks and involves high-resolution HLA typing to confirm compatibility before proceeding to donor workup and stem cell collection. For patients who cannot find a matched donor through registries, haploidentical family member donors offer a reliable alternative, as virtually every patient has at least one haploidentical family member who could serve as a donor.
Leading international BMT centers like those in Turkey have established connections with major international donor registries and can facilitate unrelated donor searches for international patients. Acıbadem Maslak Hospital maintains its own HLA typing laboratory capable of performing high-resolution molecular typing, ensuring accurate and timely donor matching. For patients with rare HLA types or from underrepresented ethnic groups, cord blood units from international cord blood banks may provide the best chance at finding a suitable graft source, and the hospital's transplant team has experience selecting and utilizing cord blood grafts for both adult and pediatric patients.
Recovery & Potential Complications
Recovery from bone marrow transplantation is a gradual and closely monitored process that typically spans several months to a year or more. The initial post-transplant period, from day zero through engraftment (usually 10 to 21 days after transplant), is characterized by severe pancytopenia, meaning the patient has very low levels of all blood cell types. During this critical period, patients require protective isolation in HEPA-filtered rooms, daily blood counts and chemistry monitoring, red blood cell and platelet transfusions, broad-spectrum antibiotics for fever and suspected infections, and intravenous nutrition when oral intake is inadequate. Engraftment, confirmed by rising white blood cell counts produced by the donor stem cells, marks the beginning of immune reconstitution.
Graft-versus-host disease is the most significant complication unique to allogeneic bone marrow transplantation. Acute GVHD typically occurs within the first 100 days post-transplant and most commonly affects the skin, liver, and gastrointestinal tract. Symptoms range from mild skin rash to severe multi-organ involvement requiring intensive immunosuppressive therapy. Chronic GVHD can develop after day 100 and may affect virtually any organ system, presenting with features resembling autoimmune conditions. Prevention strategies including calcineurin inhibitors, methotrexate, and post-transplant cyclophosphamide have significantly reduced the incidence and severity of GVHD, but it remains a major cause of morbidity and mortality after allogeneic transplant.
Infection is a constant concern throughout the post-transplant period due to the severely compromised immune system. Bacterial infections are most common during the neutropenic period before engraftment, while viral reactivations (CMV, EBV, adenovirus) and fungal infections become more prominent during the early and late post-engraftment periods as the immune system slowly reconstitutes. Comprehensive infectious disease surveillance and prophylaxis protocols at leading transplant centers like Memorial Şişli Hospital help detect and treat infections early, significantly reducing their impact on patient outcomes. Full immune reconstitution, including the ability to respond normally to vaccines and fight infections independently, typically requires 12 to 24 months after transplant.
The bone marrow transplant team in Istanbul literally gave me a second chance at life. Their expertise, dedication, and compassion throughout my treatment were beyond anything I could have imagined. Today, 18 months post-transplant, I am cancer-free and grateful beyond words.
Anna S., leukemia patient from Germany
Frequently Asked Questions
Frequently Asked Questions
How long does a bone marrow transplant take?
The actual transplant infusion takes about 1-2 hours, but the entire process from conditioning chemotherapy through initial recovery spans 4-6 weeks in hospital. Total recovery with close monitoring near the hospital typically requires 3-6 months.
What is the success rate for BMT abroad?
Success rates depend heavily on the disease, disease stage, and donor type. For common indications, leading international centers report 5-year overall survival rates of 50-80%, comparable to Western centers. Autologous transplants for lymphoma achieve 60-80% long-term survival.
How do I find a bone marrow donor?
The transplant center will first test your siblings for HLA compatibility (25-30% chance of match). If no sibling match is found, they can search international registries with 40+ million donors. Haploidentical family members offer a readily available alternative.
Can I receive a BMT if I'm over 60?
Yes, reduced-intensity conditioning protocols have extended BMT eligibility to patients in their 60s and even 70s. The suitability depends more on overall fitness and organ function than chronological age. Your transplant team will assess your fitness for transplant individually.
What follow-up is needed after returning home?
Frequent blood tests (weekly for the first 3 months, then monthly), monitoring for GVHD symptoms, infection surveillance, and medication management. Your local hematologist should receive detailed records from the transplant center and maintain ongoing communication with the international team.