Modern Colorectal Cancer Treatment
Colorectal cancer — encompassing cancers of the colon and rectum — is one of the most common cancers globally, with approximately 1.9 million new cases annually. It is also one of the most successfully treated when caught early, with Stage I colon cancer having 5-year survival rates over 90%. Even at advanced stages, the modern treatment arsenal has significantly extended survival. Comprehensive genomic profiling of colorectal tumors guides treatment selection: MSI-H/dMMR status identifies patients who respond dramatically to immunotherapy; KRAS/NRAS/BRAF mutation status determines eligibility for anti-EGFR biologics (cetuximab, panitumumab); HER2 amplification identifies a subset benefiting from HER2-directed therapy; and BRAF V600E mutations identify candidates for targeted BRAF+MEK inhibitor combinations.
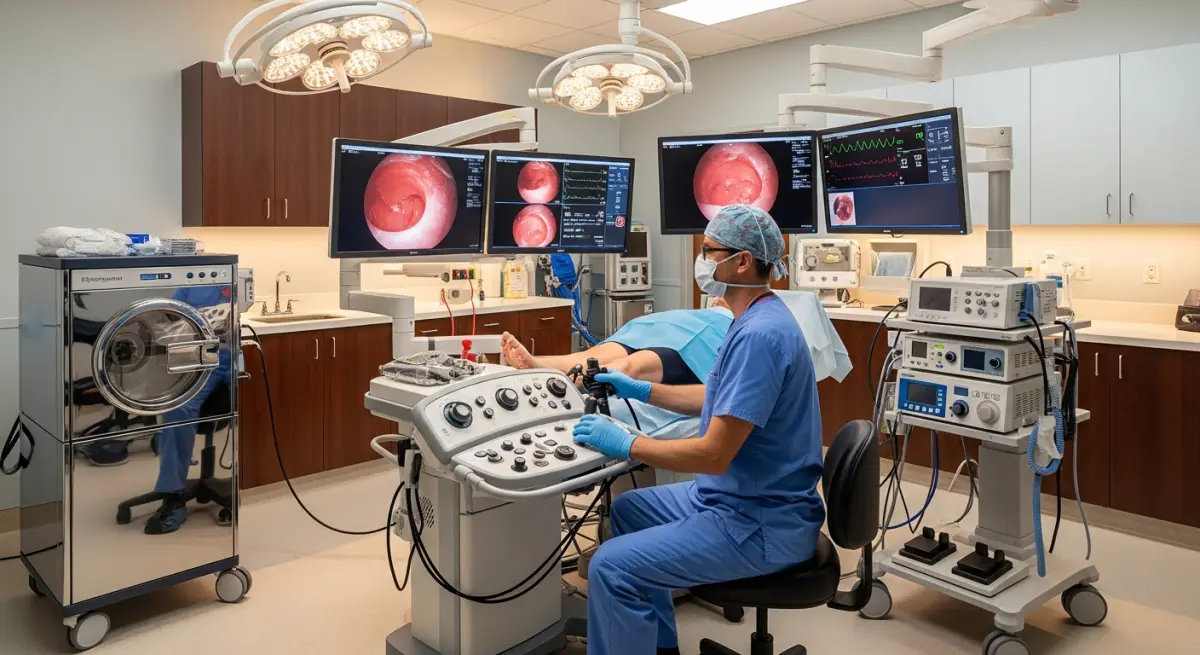
The surgical management of colorectal cancer has been transformed by minimally invasive techniques. Laparoscopic and robotic-assisted colorectal resections now represent the standard of care at high-volume specialized centers, delivering equivalent oncological outcomes to open surgery while dramatically reducing blood loss, hospital stay (typically 3–5 days versus 7–10 days for open surgery), postoperative pain, and recovery time. For rectal cancers, the da Vinci robotic system provides particular advantages in the narrow confines of the pelvis — allowing sphincter-preserving surgery in tumors previously requiring colostomy, and total mesorectal excision (TME) with unprecedented precision.
Neoadjuvant therapy (treatment before surgery) has become standard for most rectal cancers: chemoradiation or short-course radiation followed by surgery achieves tumor downstaging, increases the rate of sphincter preservation, reduces local recurrence rates, and in a proportion of patients achieves pathological complete response — allowing watch-and-wait approaches that potentially avoid surgery altogether. The international OPRA and RAPIDO trials have defined optimal neoadjuvant approaches, and these protocols are implemented at internationally accredited cancer centers including Anadolu Medical Center in Istanbul and University Hospital Cologne, both of which maintain comprehensive colorectal oncology programs with high surgical volumes and active clinical trial participation.

HIPEC for Peritoneal Metastases
Hyperthermic Intraperitoneal Chemotherapy (HIPEC) combined with cytoreductive surgery (CRS) is a specialized procedure that offers potential cure or long-term remission to selected patients with colorectal cancer that has spread to the peritoneum (the lining of the abdominal cavity). Previously, peritoneal metastases were uniformly considered terminal — systemic chemotherapy alone is poorly effective against peritoneal deposits due to the blood-peritoneal barrier. CRS+HIPEC surgically removes all visible peritoneal tumor deposits and then bathes the abdominal cavity with heated chemotherapy solution at 42°C, penetrating residual microscopic disease that surgery cannot visualize. Carefully selected patients (limited peritoneal burden, resectable disease, no other distant metastases) achieve 5-year survival rates of 25–40% with CRS+HIPEC.
CRS+HIPEC is a major, 6–10 hour operation available only at specialized high-volume centers — not at general surgical practices. Patient selection is critical: the procedure's benefit is limited to patients with peritoneal cancer index (PCI) scores below a center-specific threshold, and experienced centers have well-defined eligibility criteria. In the US, CRS+HIPEC costs $80,000–$120,000 and is available at approximately 60 centers nationally. Abroad, specialized centers in Turkey and India perform CRS+HIPEC for $18,000–$30,000 with outcomes published to international standards. Visiting centers abroad for HIPEC evaluation requires obtaining and sharing all imaging with the surgical team for detailed assessment of peritoneal burden before traveling.
Cost Comparison by Country
Colorectal Cancer Treatment Cost Comparison 2025
| Treatment | Turkey/India | South Korea/Germany | USA |
|---|---|---|---|
| Robotic Colorectal Resection | $12,000 – $22,000 | $22,000 – $40,000 | $55,000 – $90,000 |
| HIPEC + CRS Surgery | $18,000 – $30,000 | $30,000 – $55,000 | $80,000 – $120,000 |
| Chemo + Bevacizumab (cycle) | $2,500 – $5,000 | $5,000 – $9,000 | $15,000 – $25,000 |
| Pembrolizumab (MSI-H) | $2,500 – $5,000 | $5,000 – $9,000 | $15,000 – $25,000 |
| FOLFOX Chemotherapy (cycle) | $1,200 – $2,500 | $2,500 – $4,500 | $8,000 – $15,000 |
| Second Opinion Package | $500 – $1,500 | $1,000 – $2,500 | $2,000 – $5,000 |
HIPEC (Hyperthermic Intraperitoneal Chemotherapy) is a specialized procedure performed at select high-volume centers. CRS = Cytoreductive Surgery. Treatment costs depend on disease extent, protocol, and duration.
Turkey hosts several internationally accredited cancer centers with high-volume colorectal surgery programs. Anadolu Medical Center — accredited by JCI and holding ESMO and OECI designations — performs 500+ colorectal cancer operations annually and offers a comprehensive multidisciplinary approach including all molecular testing, neoadjuvant treatment, robotic surgery, and medical oncology within a single institution. The center's affiliation with Johns Hopkins Medicine provides academic collaboration and access to clinical trial protocols from the Johns Hopkins Sidney Kimmel Comprehensive Cancer Center.
South Korea's leading cancer hospitals — Asan Medical Center in Seoul and Samsung Medical Center — consistently rank among the world's highest-volume colorectal cancer surgery programs, with published outcome data showing complication rates and survival figures comparable to the world's best-performing institutions. The Korean oncology system places particular emphasis on multidisciplinary tumor board review of every case, ensuring treatment decisions are made by the collective expertise of colorectal surgeons, radiation oncologists, medical oncologists, radiologists, and pathologists simultaneously reviewing each patient's case. This team-based approach to decision-making is associated with better adherence to treatment guidelines and improved outcomes.
Access world-class colorectal cancer care abroad. Get your medical records reviewed and treatment plan developed by top oncology teams.
Request Oncology ConsultationThe Value of International Second Opinion
A second opinion from a high-volume specialized colorectal cancer center is one of the highest-value healthcare decisions a patient can make, particularly when the treatment plan involves major surgery, complex multimodality therapy, or peritoneal disease management. Studies from major cancer centers document that 20–30% of colorectal cancer second opinions result in changed recommendations — including changes in surgery type, addition or omission of neoadjuvant treatment, identification of HIPEC eligibility not recognized at the referring institution, or enrollment in clinical trials. An international second opinion can typically be obtained remotely for $500–$2,500 by submitting a complete medical record package to the center.
Get your colorectal cancer treatment plan reviewed by world-class specialists. Remote second opinions available within 1-2 weeks.
Get International Second OpinionFrequently Asked Questions
What is the difference between colon cancer and rectal cancer treatment?
While both are colorectal cancers sharing common molecular features, they differ significantly in their primary treatment approach. Colon cancers are primarily treated with surgery first (if resectable), followed by adjuvant chemotherapy for Stage III and selected Stage II cases. Rectal cancers are typically treated with neoadjuvant chemoradiation (radiation concurrent with fluoropyrimidine chemotherapy) followed by surgery and then adjuvant chemotherapy — this sequence reduces local recurrence and increases sphincter preservation rates. The distinction between colon and rectal cancers (defined by the tumor's relationship to the peritoneal reflection) is critical for correct treatment planning.
Will I need a colostomy?
The vast majority of colorectal cancers do not require permanent colostomy when treated at experienced specialized centers. Modern robotic-assisted total mesorectal excision techniques achieve sphincter preservation in 85–90% of rectal cancers when combined with effective neoadjuvant therapy for tumor downstaging. Temporary loop ileostomy (a small bowel opening used to protect low anastomoses during healing) is sometimes used and is reversed after 8–12 weeks. Only very low rectal tumors directly involving the sphincter mechanism, or cases where sphincter function cannot be preserved with acceptable continence, require permanent colostomy.
How long does colorectal cancer surgery take and what is the hospital stay?
Robotic or laparoscopic colorectal resection typically takes 2–4 hours. The hospital stay is generally 3–5 days for uncomplicated laparoscopic/robotic cases. Open surgery requires 7–10 days. CRS+HIPEC is a 6–10 hour operation with a hospital stay of 7–14 days. For international patients, plan for 10–14 days total in-country for laparoscopic/robotic surgery and 14–21 days for CRS+HIPEC, allowing for full preoperative evaluation, surgery, hospital recovery, and post-discharge wound assessment before departure.
What follow-up is required after colorectal cancer surgery abroad?
Standard colorectal cancer follow-up includes: CEA blood marker measurement every 3 months for 3 years, then every 6 months; CT chest/abdomen/pelvis every 6–12 months for 3–5 years; colonoscopy at 1 year post-surgery and then every 3–5 years. This follow-up schedule is performed at home with your local oncologist. The treating team abroad will provide comprehensive surgical and pathology reports and a specific surveillance schedule for your local physician. Remote consultation (video call) with the international treating surgeon for oncological questions is typically available throughout your follow-up period.
Is HIPEC the right treatment for my peritoneal metastases?
Patient selection for HIPEC is complex and must be individualized. Key factors determining eligibility include: peritoneal cancer index score (PCI) from CT imaging — generally PCI ≤20 for colorectal cancer; absence of extra-abdominal metastases; adequate liver and kidney function; resectability of all peritoneal deposits (R0 or R1 resection achievable); and patient fitness for major surgery. Patients with synchronous liver metastases may still be HIPEC candidates in select circumstances. The best way to determine HIPEC eligibility is to have your CT imaging reviewed by a high-volume HIPEC surgeon — this can be done remotely through a second opinion consultation.